Here are some select resources to help our patients with cancer and hematological disorders in their disease management
Find Clinical Trials
Cancer Patient Support Groups
Medication Assistance
Cancer Management Guidelines
Common Hematological Conditions
Educational Videos
Here is a small compilation of videos that are from online sources such as youtube. These are for educational purpose alone and do not constitute medical advice.
-
Staging cancers: TNM and I-IV systems
Staging cancers is important to determine the prognosis of a patient and what treatment they might best benefit from. It is also vital to structuring research and developing guidelines for cancer treatment.
The most widely used system is the TNM system. T stands for tumour, and gives an impression of how large, or how locally invasive the primary tumour is.
N stands for node. This refers to the number of lymph nodes close to the tumour that are affected.
M stands for Metastases. If a tumour has spread and begins to form secondary tumours in other parts of the body it is said to have metastasised.
The number system (Stage I-IV) integrates information from the TNM system to come up with a simplified score.
References
http://cancerstaging.org/references-tools/Pages/What-is-Cancer-Staging.aspx -

IMMUNOTHERAPY: The Path to a Cancer Cure (For Clinicians)
Created by Dr. Samir N. Khleif (Georgetown Lombardi Comprehensive Cancer Center), in partnership with the Society for Immunotherapy of Cancer (SITC) and Cancer Support Community, IMMUNOTHERAPY: The Path to a Cancer Cure explains the interplay between the immune system and cancer; mechanisms underlying immune-based agents; and different approaches to cancer immunotherapeutics.
Patients: Watch the Patient version of this video here: https://www.youtube.com/watch?v=afdq8Op-jQM -
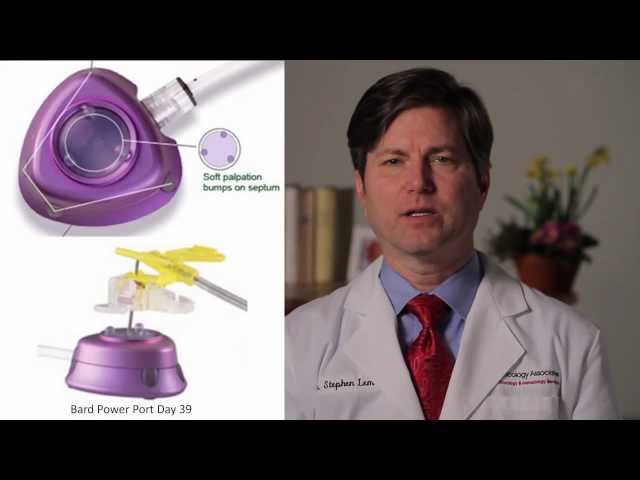
How a Portacath is used for Chemotherapy Treatment
Oncologist Dr. Stephen Lemon from Oncology Associates in Omaha, Nebraska explains how a port-a-cath is used for cancer treatment during chemotherapy. Visit http://oacancer.com/patient-info/resources/video/medical-minutes/ to watch more videos on cancer treatment.
Medical Minute cancer information videos are produced by Dr. Stephen J. Lemon, who is a medical oncologist who now works with the Overlake Cancer Center in Bellevue, WA. These videos were produced to provide useful cancer information to cancer patients and survivors. Visit https://www.canceris.net/ to find and share more cancer information.
Oncology Associates provides a full range of personalized cancer care at two Omaha clinics as well as at cancer treatment clinics throughout Nebraska.
The physicians of Oncology Associates include:
* Irina E. Popa, MD
To learn more about OA's approach to personalized cancer treatment as well as about the oncologists and staff, please visit http://www.oacancer.com
Video Transcript:
Using a portacath during chemotherapy – Dr. Stephen Lemon
Portacaths, or ports, are vascular access devices used for the treatment of chemotherapy that is given intravenously.
Portacaths sit under the skin and the catheter goes into a large vein. This helps in the chemotherapy administration, and can also be used to draw blood for blood counts and blood tests. This is also a safe way to give chemotherapy, with less chance of the chemotherapy leaking out of the vein and causing damage to skin or other tissues.
The portacath, shown here, is accessed with a needle that goes through the skin and into the portacath chamber. So blood fills the chamber, and can be withdrawn through the needle to have blood tests done before chemotherapy. And then at the time of chemotherapy treatment the chemo drug is given through the needle into the chamber, and then into the vein through the catheter.
At the completion of your chemotherapy treatment the needle will be removed from the port and from the skin so that when you go home there isn't any needle or any catheters or anything that requires care. Simply keep the skin clean and dry.
Once a patient's cancer treatment is completed and they no longer require chemotherapy, the portacath can be removed as a simple outpatient procedure. Sometimes your doctor may ask you to keep the portacath in for a little bit longer in case of additional blood draws or possible additional treatment.
If a portacath is going to be maintained after the completion of cancer treatment it needs to be flushed once a month to prevent blood clots from forming in the catheter.
To watch more videos visit http://www.canceris.net and http://www. oacancer.com. -
What are ‘targeted’ cancer drugs? | Cancer Research UK
This video explains the concept of so-called 'targeted' cancer drugs, built from a fundamental undertanding of the shape and function of the faulty molecules inside cancer cells. Find out more about our work on cancer drugs here: http://bit.ly/1DfoCuq and read about how faults in the BRAF gene were linked to cancer by Cancer Research UK-funded scientists on our blog: http://bit.ly/1L77hbt -

PET-Imaging
Describes how the PET-CT scanner can help us find cancers in the body -

Hormonal Therapy for Breast Cancer: We Teach You
We teach you about hormonal therapy for breast cancer. Drugs such as tamoxifen and aromatase inhibitors are key treatment options for most breast cancers.
VISIT THE BREAST CANCER SCHOOL FOR PATIENTS:
http://www.breastcancercourse.org
LIST OF QUESTIONS FOR YOUR DOCTORS:
http://www.breastcancercourse.org/breast-health-updates-latest-videos/
FOLLOW US:
Facebook: https://www.facebook.com/Breast-Cancer-School-for-Patients-958519147618444/
________________________________
Questions for your Medical Oncologist:
1. What type of hormonal therapy do you recommend?
2. Will I also benefit from chemotherapy?
3. What are the side effects of hormonal therapy?
4. Will I need 5 or 10 years of these medications?
5. Would the genomic assay Oncotype DX be helpful?
6. What is Hormonal Therapy?
Anti-estrogen (estrogen-blocking) medications, prescribed as pills, are incredibly effective at treating certain types of breast cancer. Hormonal therapy is given to about 70 to 80% of women with breast cancer. Chemotherapy, on the other hand, is a more intense cancer treatment that is generally administered intravenously. Most patients will not need chemotherapy. Many women that do need chemotherapy will also benefit from hormonal therapy. These treatment decisions are complex ones with your medical oncologist. You will make better choices when you are well informed before meeting with your medical oncologist.
Do my “Receptors” suggest Hormonal Therapy?
When the estrogen circulating in your blood stream interacts with a breast cancer that has “Estrogen Receptors” (ER) present on its surface, it tends to flip the ER switch to the “on” or “grow” position for ER Positive tumors. The same can be said to a lesser extent for the “Progesterone Receptor,” if your cancer is found to also be PR positive. Patients with ER+ breast cancers almost always benefit from the anti-estrogen effects of hormonal therapy. These medications can make cancer cells die, or slow down their growth. If a few cancer cells have already spread to other parts of the body, these medications are incredibly effective at preventing these cells from growing and threatening your life in the future. In other words, those who take hormonal therapy for ER+ tumors have a more successful chance at long-term survival when compared to those who do not.
About 80% of all breast cancers are ER+. Even if your medical oncologist recommends chemotherapy for you, if your tumor is ER+ you will also benefit from up to 10 years of hormonal therapy after chemotherapy. Hormonal therapy is never given during chemotherapy nor during radiation therapy.
What is “Tamoxifen?”
Tamoxifen is an anti-estrogen medication (pills) that has been used with great success with ER+ cancers for three decades. It is now the primary hormonal therapy for younger, pre-menopausal women. It is also the primary drug for men with breast cancer. It is used for some post-menopausal women.
What are “Aromatase Inhibitors?”
Aromatase inhibitors (AIs) are a class of anti-estrogen medications (pills) that have proven to be slightly more effective than Tamoxifen for post-menopausal women. It is not recommended for younger, pre-menopausal women, except in certain circumstances. The three most common versions are Anastrozole (Arimidex), Letrozole (Femara), and Exemestane (Aromasin).
What are the side effects of Hormonal Therapy?
Side effects vary greatly from one person to the next for both types of hormonal medications. Some have no symptoms at all. Most have very tolerable side effects. Some patients will need to change hormonal therapy medications to find the best balance of cancer benefit versus side effects. Several side effects that are rather common for both tamoxifen and aromatase inhibitors are hot flashes, night sweats, joint pain, and vaginal dryness. Below, we list some of the other specific side effects for both drugs.
Tamoxifen Side Effects:
Increased risk of uterine (endometrial) cancer
Increased risk of developing blood clots
Slows normal bone loss in most women (a “good” side effect)
Cannot be taken during pregnancy because of risk of birth defects or fetal death
Can temporarily induce menopause in pre-menopausal women.
Aromatase Inhibitor Side Effects:
Can worsen bone loss (osteoporosis) in women
Muscle and joint aches and pains
Would an “Oncotype DX” assay help me?
Patients who have a small, estrogen receptor positive, HER2 receptor negative tumor, and no evidence of cancer in their lymph nodes may benefit from an Oncotype DX genomic assay. This cutting-edge test looks deeper into your cancer cells to better identify people who may also benefit from chemotherapy with ER+ breast cancers. The decision to undergo chemotherapy, in addition to hormonal therapy, is a complicated one. Your medical oncologist uses many factors to help decide if you will benefit from chemotherapy. An Oncotype DX analysis of a portion of your breast cancer tissue can be instrumental in this decision. -

How a Linear Accelerator works – Elekta
Have you ever wondered how a linear accelerator works and what it does?
A linear accelerator is a device that produces a beam of either electrons or very high energy X-rays that can be used to treat cancer. In this video, you will see an Elekta Synergy, an accelerator that is used for radiation therapy.
Radiation therapy is a treatment that uses high-energy radiation to kill cancer cells or shrink tumors. The radiation beam can be shaped and directed to match the tumor shape, so that it can target the cancer cells while sparing the healthy tissue. The beam of radiation is delivered with an accuracy of 2mm, which means that it can hit the tumor precisely and avoid damaging the surrounding organs.
How does a linear accelerator shape and direct the radiation beam?
There are three ways to do that:
- Using the primary and secondary collimators. These are large tungsten blocks that can shape the X-ray beam into the appropriate square shape.
- Using custom blocks. These are cast blocks that are made specifically for an individual patient to shield sensitive tissue or structures. They can be made to the exact shape of the tumor.
- Using a Multileaf Collimator (MLC). This is a device that has fine leaves (usually 1cm wide) that are computer-controlled to move in and out of the X-ray beam. The MLC can create complex shapes that match the tumor shape. This is the most common method used in many countries.
If you want to learn more about how a linear accelerator works and what it does, watch this video and visit the Elekta website here:
https://www.elekta.com/products/radiation-therapy/?utm_source=youtube&utm_medium=YT-description&utm_content=&utm_campaign=YT-CT-Linac-Radiation
or watch this playlist:
https://www.youtube.com/playlist?list=PL18C46063BA30078D
Discover how this amazing technology can help improve the quality of life for cancer patients.
For any inquiries or to learn more about how Elekta can support you, please contact us here:
https://www.elekta.com/contact/?contact_source=YT-CT-Linac-Radiation
Receiving Radiosurgery treatment?
Additional information for patients can be found on our website:
https://www.elekta.com/patients/radiation-therapy-treatment/?utm_source=youtube&utm_medium=YT-description&utm_content=&utm_campaign=YT-CT-Linac-Radiation
For everything else, including videos on different types of treatments, machines, thought leadership and more, subscribe to our channel and head over to our website!
https://www.elekta.com/products/radiation-therapy/?utm_source=youtube&utm_medium=YT-description&utm_content=&utm_campaign=YT-CT-Linac-Radiation
#radiationtherapy #oncology
Chapters:
00:00 Introduction: How a linear accelerator works
00:42 How the X-ray Beam is generated and shaped
04:42 How the radiation dose is measured and controlled
06:17 How the Linac is operated and monitored
07:11 Clearance -

What is radiotherapy and how does it work? | Cancer Research UK
Radiotherapy plays a crucial part in treating lots of different cancers. And new technology is making it more precise and reducing side effects. It works by firing x-rays or other intense bundles of energy at cancer cells, damaging their DNA. If a cancer cell can't repair its damaged DNA, it dies.
0:01 Radiotherapy
0:20 What does the radiation do?
0:30 How does radiotherapy work?
1:04 SABR - a new technique
1:24 Proton beam therapy
1:42 Thyroid cancer treatment
Find out more about radiotherapy on the Cancer Research UK news website: https://news.cancerresearchuk.org/series/radiotherapy/
Subscribe: youtube.com/user/cancerresearchuk
Facebook: facebook.com/cancerresearchuk
Twitter: twitter.com/CR_UK
Instagram: instagram.com/cr_uk -

What Are Clinical Trial Phases?
Watch to learn about the three main phases of clinical trials. Clinical trials are research studies that involve people. Understanding what they are can help you decide if a clinical trial might be an option for you or a loved one.
_______________________________________
For more on clinical trials, visit: https://www.cancer.gov/clinicaltrials
To find NCI-supported clinical trials, go to: https://trials.cancer.gov
Need help finding a trial? Have a cancer-related question? Call, e-mail, or write the NCI Contact Center at: https://www.cancer.gov/contact
_______________________________________
Clinical trials are research studies that involve people. Most clinical trials to test new cancer treatments are done in a series of steps, called phases. If a new treatment is successful in one phase it moves to the next phase. Let's take a look at the three main phases of clinical trials. Phase 1 trials are small enrolling less than thirty patients. Phase 1 trials are designed to find a safe dose of the new treatment, determine how the treatment should be given, and learn how it affects the body. If a safe doses found the new treatment goes to phase 2 testing. More patients are enrolled, usually 100 or less. Phase 2 trials study have the treatment effects the body, and how the treatment works for a certain type of cancer. If a new treatment is found to be safe and have some benefit, it goes to phase 3. This is when many participants are needed, usually more than 100 and sometimes thousands. Phase 3 trials compared the new treatment with the current treatment to see which one is better. One thing is certain with any phase trial, by taking part you will help future patients by helping today's scientists learn more about cancer. For more information about clinical trials, including their possible risks and benefits for you go, to cancer.gov/clinicaltrials -

What are antibody-drug conjugates and how do they work against cancer?
A challenge of cancer treatment is doing our best to ensure that the benefits a medicine brings outweigh the burden of unwanted side effects. Chemotherapy, for example, is a powerful treatment that kills cancer cells, but it damages healthy cells too, leading to side effects like hair loss and tiredness. Monoclonal antibodies are also used to treat cancer and are capable of a more targeted attack on tumour cells.
What if we could combine the targeting power of monoclonal antibodies and the toxic properties of chemotherapy to help the treatment to selectively kill cancer cells? That’s where antibody-drug conjugates (ADCs) come in.
http://www.roche.com/antibody-drug_conjugates
More videos on http://www.youtube.com/user/roche -

What is Precision Medicine?
Precision medicine involves unraveling your genetic code to find the exact best care for your cancer and developing treatments that perfectly fit you.Two people may have the same type of cancer, but one individual's cancer may grow and spread differently than the other's. Even though cancer treatments have greatly improved, no two people respond to treatment exactly alike. Treatments need to be custom-fit to each person. Precision medicine links the fields of genetics, biology, and medicine to tailor treatment plans specifically to each patient. At Henry Ford Health System in Detroit, we believe your cancer care should be as personalized as a fingerprint. Learn more about precision medicine at https://www.henryford.com/services/cancer/treatments/precision-medicine. -

Liquid biopsies to monitor cancer
Being able to easily track cancer is vital in all stages of the disease. Doctors have long been able to monitor the disease with scans and by taking small tissue samples (biopsies), but now a new technique is becoming available to them: the liquid biopsy, which can deliver a lot of detailed information about a patient's tumour from a simple blood sample.
So how does it work? Inside a tumour, cells are growing at a high rate, but while many cancer cells are growing, some are also dying in a process called apoptosis. As dying cancer cells break up, they release fragments of their DNA. Some of that DNA can get into the blood stream, after which it's called circulating tumour DNA (or ctDNA). This circulating tumour DNA is ready for scientists to fish out with a simple blood sample.
Because of advances in DNA sequencing technology, doctors can pick up on these traces of DNA, and use them to track the mutations present in a cancer. Finding out this information helps doctors keep track of a patient's tumour and whether treatment is working, or find out early if a new scan or different treatment is needed.
For more information, see
http://scienceblog.cancerresearchuk.org/2016/12/20/searching-for-a-blood-test-to-monitor-ovarian-cancer/
http://scienceblog.cancerresearchuk.org/2016/03/15/blood-analysis-could-offer-a-real-time-snapshot-of-melanoma-treatment/


